What is genetic testing?
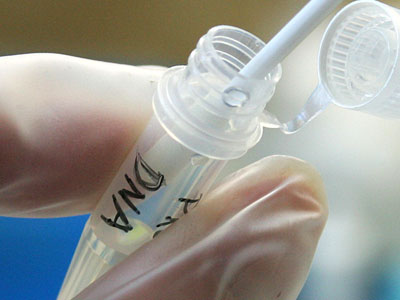
Genetic testing is a medical test that identifies changes in chromosomes, genes, or proteins. The results of a genetic test can confirm or rule out a suspected genetic condition or help determine a person's chance of developing or passing on a genetic disorder. More than one thousand genetic tests are currently in use, and many more are being developed.
Gene tests look for signs of a disorder or disease in DNA or RNA, and chromosomal tests look at features of a person's chromosomes, including their structure, number and arrangement. Biochemical tests look at the amounts or activities of key proteins. Since genes contain the DNA code for making proteins, abnormal amounts or activities of proteins can signal genes that are not working normally. These types of tests are often used for newborn screening, for example biochemical screening can detect infants who have metabolic conditions such as phenylketonuria.
Genetic testing is a medical test that identifies changes in chromosomes, genes, or proteins. The results of a genetic test can confirm or rule out a suspected genetic condition or help determine a person's chance of developing or passing on a genetic disorder. More than one thousand genetic tests are currently in use, and many more are being developed.
Gene tests look for signs of a disorder or disease in DNA or RNA, and chromosomal tests look at features of a person's chromosomes, including their structure, number and arrangement. Biochemical tests look at the amounts or activities of key proteins. Since genes contain the DNA code for making proteins, abnormal amounts or activities of proteins can signal genes that are not working normally. These types of tests are often used for newborn screening, for example biochemical screening can detect infants who have metabolic conditions such as phenylketonuria.
What information does genetic testing give?
Genetic testing can:
Genetic testing can:
- Give a diagnosis if someone has symptoms.
- Show whether a person is a carrier for a genetic disease. Carriers have an altered gene, but will not get the disease. However, they can pass the altered gene on to their children.
- Help expectant parents know whether an unborn child will have a genetic condition. This is called prenatal testing.
- Screen newborn infants for abnormal or missing proteins that can cause disease. This is called newborn screening.
- Show whether a person has an inherited disposition to a certain disease before symptoms start.
- Determine the type or dose of a medicine that is best for a certain person. This is called pharmacogenetics.
What is in vitro fertilisation?
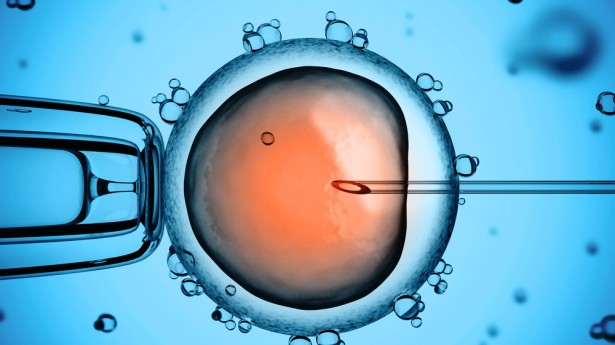
In vitro fertilisation, short for IVF, is a treatment that involves the fertilisation of an egg (or eggs) outside the body. The treatment can be performed using a couple's eggs and sperm, or by donated eggs and sperm. IVF is a form of assisted, reproductive technology, and it uses special, medical techniques to allow a woman to be pregnant. After having manually fused a woman's egg and a man's sperm in a laboratory dish, a speculum is inserted into the woman's vagina, which holds the cervix open and therefore allows a fine tube (known as catheter) to be passed through the cervix using ultrasound for guidance. Then, the embryos are passed down the tube and into the womb. In the UK, if you are under 40, you can place one or two embryos in the womb, to enhance your chance of success of becoming pregnant. If you are over 40, you are allowed to place up to three embryos in your womb, where, in most situations, you will be left with one alive embryo which will become your baby. By using IVF, the percentage of a woman becoming pregnant is 20-35%, however women with top chances of success with IVF will receive a percentage of 40%.
In vitro fertilisation, short for IVF, is a treatment that involves the fertilisation of an egg (or eggs) outside the body. The treatment can be performed using a couple's eggs and sperm, or by donated eggs and sperm. IVF is a form of assisted, reproductive technology, and it uses special, medical techniques to allow a woman to be pregnant. After having manually fused a woman's egg and a man's sperm in a laboratory dish, a speculum is inserted into the woman's vagina, which holds the cervix open and therefore allows a fine tube (known as catheter) to be passed through the cervix using ultrasound for guidance. Then, the embryos are passed down the tube and into the womb. In the UK, if you are under 40, you can place one or two embryos in the womb, to enhance your chance of success of becoming pregnant. If you are over 40, you are allowed to place up to three embryos in your womb, where, in most situations, you will be left with one alive embryo which will become your baby. By using IVF, the percentage of a woman becoming pregnant is 20-35%, however women with top chances of success with IVF will receive a percentage of 40%.
Many couples use in vitro fertilisation to produce babies for several different reasons. The couple may be unable produce babies of their own, for example the woman's fallopian tubes may be blocked, or the man or woman may have been diagnosed with unexplained infertility, however a great proportion of couples who use in vitro fertilisation to produce babies perform this act because they do not want to pass on a genetic disease onto their children.
How do genetic testing and in vitro fertilisation link?
Many couples who want to produce a baby, will visit the doctors before they are about to do so. Here, the couple will check for any sexually transmitted diseases that they could contain, and they will perform a genetic test which will inform the male and female whether there could be a risk of their child receiving a genetic disease. An extremely common example of this disease is cystic fibrosis, which is an inherited genetic disorder. this disease affects the lungs and digestive system by clogging them up with thick, sticky mucus. This makes it difficult to breathe and digest food properly, which means that people with cystic fibrosis need to have daily treatment such as physiotherapy, to help clear the mucus from the lungs and antibiotic medication to fight chest infections. Many couples who have the risk of producing a child with a genetic disease tend to use IVF from a donor in order to conceive a child who will not have any risk of receiving a genetic disease. This, therefore, causes the embryo to be created outside the mother's womb, and away from its normal production route.
However, is it morally right to create babies outside a woman's womb, and it is morally right to reproduce by using a different method that God didn't intend? Is it morally right to destroy the common notions of parenthood by producing a baby with the help of doctors and laboratory technicians? Furthermore, by using IVF, should parents be allowed to choose the gender (which they are allowed to do because the sperm is specifically chosen when combined with the egg) of their child by this specific treatment? Is it morally right to do so? Surely reproduction should take place in the way that God intended it to happen? Additionally, by creating more than one embryo in a laboratory dish with the likelihood of only one surviving are we effectively creating babies and then killing them in the hope that one will survive to become a surviving foetus?
Throughout this website, I will we discussing whether it is morally right to use in vitro fertilisation, discussing several factors and key information, from the different view of four philosophers, Jeremy Bentham, Immanuel Kant, Joseph Fletcher, and Thomas Aquinas. At the end, I will explain my thoughts on in vitro fertilisation, and you too can comment and vote on your opinion!
How do genetic testing and in vitro fertilisation link?
Many couples who want to produce a baby, will visit the doctors before they are about to do so. Here, the couple will check for any sexually transmitted diseases that they could contain, and they will perform a genetic test which will inform the male and female whether there could be a risk of their child receiving a genetic disease. An extremely common example of this disease is cystic fibrosis, which is an inherited genetic disorder. this disease affects the lungs and digestive system by clogging them up with thick, sticky mucus. This makes it difficult to breathe and digest food properly, which means that people with cystic fibrosis need to have daily treatment such as physiotherapy, to help clear the mucus from the lungs and antibiotic medication to fight chest infections. Many couples who have the risk of producing a child with a genetic disease tend to use IVF from a donor in order to conceive a child who will not have any risk of receiving a genetic disease. This, therefore, causes the embryo to be created outside the mother's womb, and away from its normal production route.
However, is it morally right to create babies outside a woman's womb, and it is morally right to reproduce by using a different method that God didn't intend? Is it morally right to destroy the common notions of parenthood by producing a baby with the help of doctors and laboratory technicians? Furthermore, by using IVF, should parents be allowed to choose the gender (which they are allowed to do because the sperm is specifically chosen when combined with the egg) of their child by this specific treatment? Is it morally right to do so? Surely reproduction should take place in the way that God intended it to happen? Additionally, by creating more than one embryo in a laboratory dish with the likelihood of only one surviving are we effectively creating babies and then killing them in the hope that one will survive to become a surviving foetus?
Throughout this website, I will we discussing whether it is morally right to use in vitro fertilisation, discussing several factors and key information, from the different view of four philosophers, Jeremy Bentham, Immanuel Kant, Joseph Fletcher, and Thomas Aquinas. At the end, I will explain my thoughts on in vitro fertilisation, and you too can comment and vote on your opinion!